Category: Research
LCOH-UC study: Spinal cord stimulation a potential new way to treat depression
Lindner Center of HOPE, UC researcher publishes pilot study showing feasibility of method
A pilot clinical trial led by Lindner Center of HOPE Research Institute and University of Cincinnati researchers at the Lindner Center of HOPE found electrical stimulation of the spinal cord is feasible, well-tolerated, and shows therapeutic potential to treat depression.
The results of the trial were published in the journal Molecular Psychiatry on Dec. 20. View link at https://rdcu.be/dt41x
Research background
 Principal investigator Francisco Romo-Nava, MD, PhD, said his research focuses on how brain-body communication is involved in psychiatric disorders.
Principal investigator Francisco Romo-Nava, MD, PhD, said his research focuses on how brain-body communication is involved in psychiatric disorders.
“We think that the connection between the brain and the body is essential for psychiatric disorders,” said Romo-Nava, Associate Chief Research Officer for the Research Institute at the Lindner Center of HOPE, Associate Professor in the Department of Psychiatry and Behavioral Neurosciences at UC, and a UC Health physician scientist. “Many of the symptoms of mood disorders or eating disorders or anxiety disorders have to do with what one could interpret as dysregulation in this brain-body interaction.”
Romo-Nava said pathways of neurons located in the spinal cord convey information from the body to regions of the brain that are involved in the emotional experience we know as mood. When functioning properly, the brain uses this information to constantly make adjustments to help regulate a person’s mood.
While major depressive disorder can have many different causes, one contributor could be this pathway being overloaded with information.
“For example, chronic stress could lead to a hyperactive brain-body circuit that eventually burns the system out and prevents it from adjusting itself in an effective and optimal way,” Romo-Nava said.
The research team looked at different ways to modulate this interaction between the brain and body and developed a novel approach through non-invasive spinal cord stimulation. Romo-Nava received a patent for the device obtained a patent in 2020 for the stimulation method used after working with UC’s Office of Innovation.
The spinal cord stimulation is designed to decrease the flow of information in the brain-body circuit so that the brain is better able to readjust and regulate itself.
“Spinal cord stimulation is thought to help the brain modulate itself as it should by decreasing the noise or decreasing the hyperactive signaling that may be in place during a depressive syndrome,” Romo-Nava said.
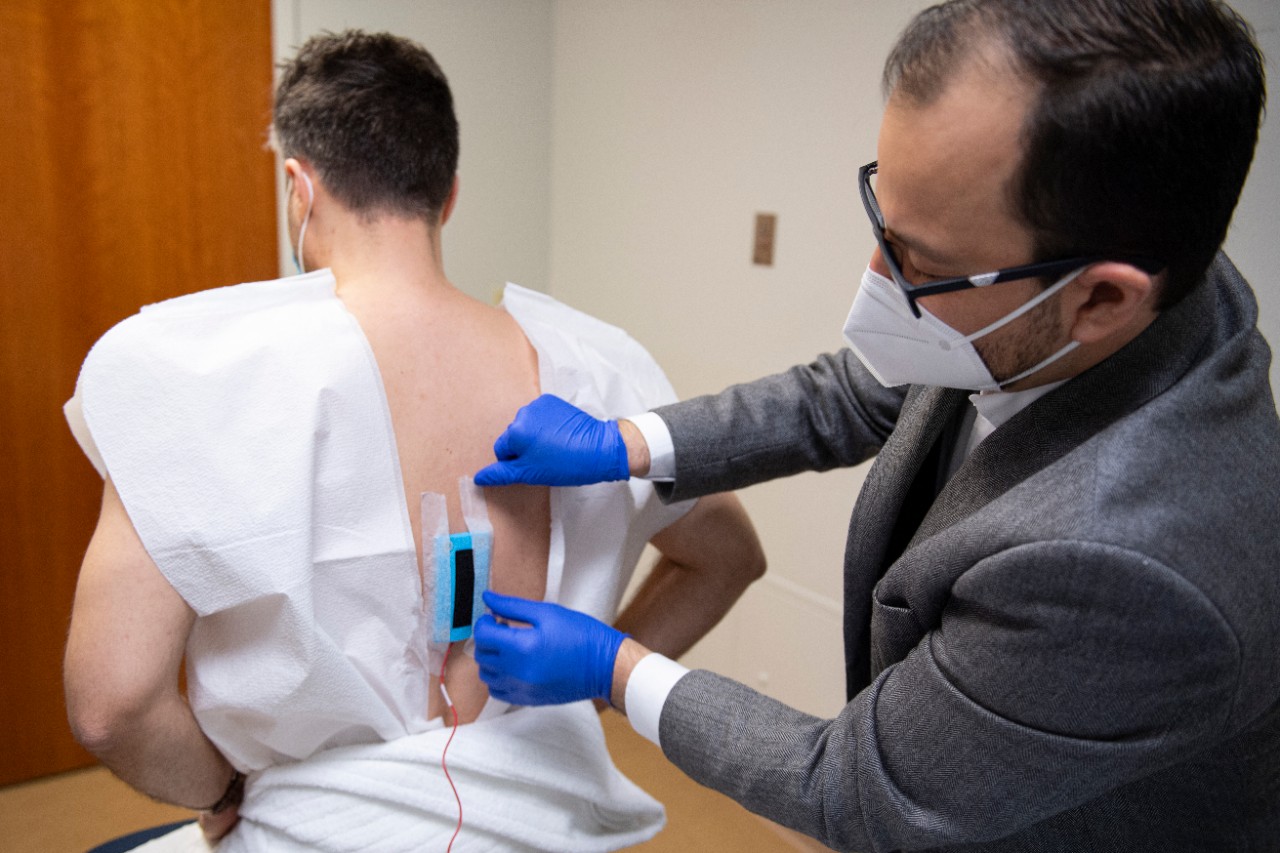
The investigational device that was used is no larger than a shoe box, with the active electrode placed on the patient’s back and the return electrode placed on their right shoulder.
Trial details
With funding through a Brain & Behavior Research Foundation NARSAD Young Investigator Award, Romo-Nava designed the pilot study to test the feasibility and tolerability of spinal cord stimulation for patients with major depressive disorder.
A total of 20 patients were enrolled in the trial, with half randomized to receive the active version of the spinal cord stimulation and half receiving a different version of current that was not expected to have much of an effect.
Patients went to the Lindner Center of HOPE for three 20-minute sessions a week for eight weeks, for a total of 24 spinal stimulation sessions.
Trial results
Romo-Nava said like with most pilot studies, the primary focus of the study was the feasibility and safety of the intervention and how well patients tolerated the stimulation. The study was designed so that the dose of stimulation could be decreased if needed, but Romo-Nava said all patients tolerated the initially prescribed dose well.
“We used a current that is so small that it’s about 10 times smaller than the one known to induce tissue damage, so that’s also pretty encouraging because there’s a lot to explore in terms of what is the optimal dose and session frequency,” he said.
Side effects of the treatment were mild, including skin redness at the site of stimulation and brief non-painful itching or burning sensations that only lasted during the treatment sessions. The skin redness typically did not last more than 20 minutes after a session, Romo-Nava said.
A virtual reconstruction of how the current from the device moves through the body showed the current reaches spinal gray matter in the spinal cord, but does not reach the brain itself.
“That supports our hypothesis that it is the modulation of these pathways of information that then may induce an effect on the mood-relevant areas in the brain,” he said. “So it is not the current that reaches the brain, it is the change in the signal that then has an effect. This study is not sufficient to prove all of these components of the hypothesis, but we think it’s a great start.”
Patients that received the active stimulation had a greater decrease in the severity of their depressive symptoms compared to the control group, but Romo-Nava cautioned the study was limited by its small sample size. These results will need to be replicated in much larger studies to be confirmed.
“We need to be cautious when we interpret these results because of the pilot nature and the small sample size of the study,” he said. “While the primary outcome was positive and it shows therapeutic potential, we should acknowledge all the limitations of the study.”
Data showed participants’ resting blood pressure did not change over the course of the eight weeks, but their diastolic blood pressure (the bottom number of a blood pressure reading) decreased for a short time after each session in a cumulative way during the study.
“That may mean that we may be actually inducing a form of plastic effect on the brain-body interaction circuit that is also involved in autonomic functions like blood pressure and heart rate,” Romo-Nava said. “This is very preliminary, but it is also another signal that is in the right direction.”
Moving forward, Romo-Nava said the research team is seeking additional funding to put together an expanded trial and develop a portable version of the spinal cord stimulation device. If further studies confirm the stimulation is safe and effective to treat psychiatric disorders, future work will also be needed to find the optimal dose, frequency and conditions it can be used for.
Lindner Center of HOPE provides excellent, patient-centered, scientifically advanced care for individuals suffering with mental illness. A state-of-the-science mental-health center and charter member of the National Network of Depression Centers, the center provides psychiatric hospitalization and partial hospitalization for adults, outpatient services for all ages, diagnostic and short-term residential services for adults, intensive outpatient program for substance abuse and co-occurring disorders for adults and research. The center is enhanced by its partnership with UC Health as its clinicians are ranked among the best providers locally, nationally and internationally. Together Lindner Center of HOPE and UC Health offer a true system of mental health care in the Greater Cincinnati area and across the country. The center is also affiliated with the University of Cincinnati (UC) College of Medicine.
##